The Last Journey: Looking at Death in Taiwan
My research is to study the form of “good death” and its significance for modern people by looking at how various concepts and customs surrounding death have appeared in the modern society where medical technologies have been highly progressed. I focus mainly on East Asian countries, especially comparing the view of life and death and the legalization of terminal care between Japan and Taiwan.
In Taiwan, there exists a custom of discharging moribund patients from the hospital and send them home by private ambulance so they can spend their end of life at home. Such custom, based on the advance wishes of the patients themselves or the surrogate decision by their family members, is called “terminal discharge.” There are also legal regulations relating to it so that death of the discharged patients at home would be treated as unsuspicious death (see Note1). This custom, so called “the last journey” or “to keep the last breath” in general, relates to the traditional concept of “dying in one's own bed at a ripe old age,” which regards dying at home as “good death” and is one of the characteristics of Taiwanese view towards life and death. For Taiwanese people, “dying in a foreign land” is a sad incident because they believe that the soul of the deceased would thus lose their way home and could not come back to join their ancestors. Therefore, when patients are in critical condition at the hospital, instead of staying and dying there, the custom of sending them home while they are still breathing and letting them die at home came to practice.
In Taiwan the National Health Insurance was introduced in 1995 and the medical system has been reorganized. As the universal medical care system is in operation, the existence of the custom of terminal discharge can be considered as an integration of medical technologies and traditional views of life and death. Such cultural background may seem to be the possible explanation of the fact that the rate of death at home in Taiwan has been higher than that in Japan. However, for the last few years the rate of death at medical institutes has been increasing in Taiwan. As Figure 1 shows, the number of persons who die at home used to account for over half of the total, but, in 2008 the number accounted for less than half of the total. In 2012 the number of persons who die at medical institutes was more than that of persons who die at home. One factor of this change is the legalization concerning terminal care. The “Hospice and Palliative Care Act,” which regulates the refusal of life-support treatment by advance directives of the patients themselves or proxy decisions made by their family members, came into effect in 2000 (see Note 2). After several revisions of the act, now the advance directives concerning life-support treatments at end of life can be stored in the database of the National Health Insurance, and patients' wishes of end-of-life care can be confirmed by simply reading the IC insurance card (see Figure 2). In cases when patients prefer hospice care rather than life-support treatment, after receiving hospice care at the hospital, some are discharged so to die at home, and others stay at the hospital and die there. What “good death” means varies from person to person, However, the purpose of the legalization is to fill in the gap of end-of-life care between places they die such as at home or at the hospital, and to respect the wishes of patients.
I would like to clarify how the issue of death has been dealt with, and what kind of impacts and lessons have the discussions and research over death brought about in East Asian countries. The theme of “death” was once regarded as a taboo in Taiwanese society, and people have tended not to discuss this topic. Family members used to follow the traditional custom and patients died at home as a tacit agreement between dying patients and their family. As the legalization of terminal care is implemented, nowadays patients come to write down their wishes in words in advance. The contents of those tacit agreements have thus become clear and patients now choose their own end of life in advance. Based on the actual situation of the custom of death and its changes, I look at death through the examination of the transformation of “good death” in Taiwan and East Asia. Through the examination of “death,” the subject of life” and “living” will become another focus for me to think of.
Note 1 Section 2, article 52 of the Medical Law in Taiwan stipulates that in case patients refuse life-support treatment and prefer death at home, they can leave the hospital by signing the document of such wishes by patients themselves or their family members.
Note 2 Chung, Yicheng “Debates on end-of-life care and the legalization of ‘natural death' in Taiwan: the practice of terminal discharge and the Hospice and Palliative Care Act,” Journal of the Japan Association for Bioethics, Vol., 23, No. 1, pp. 115 – 124, 2013
Figure 1 Yearly Transition of Component Ratio (%) of Where People Die for the Past 20 Years (1993~2012)in Taiwan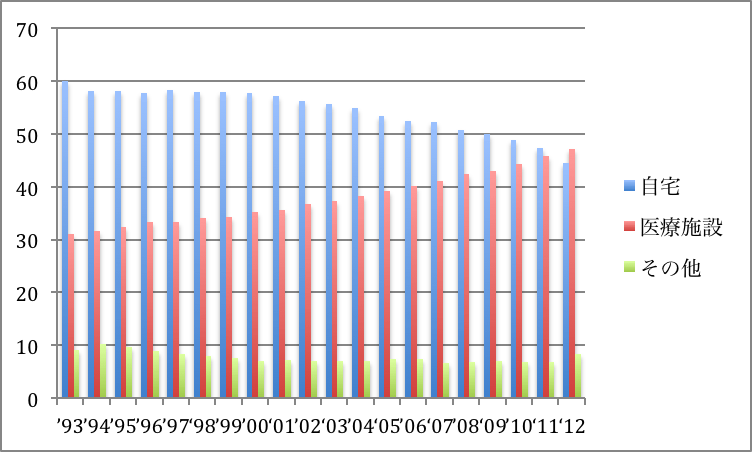
Figure 2 National Health Insurance Card and Preference Card for Hospice Care in Taiwan
CHUNG Yicheng











